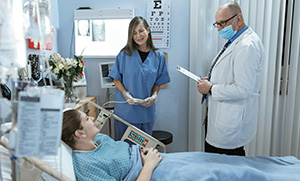
Denial Management
Denial Management
Denial management can be difficult and time-consuming, but with Precision Billing Team , you can be certain that your denied claims are in good hands. Our team of specialists is familiar with the most recent best practices for denial management and has a track record of assisting healthcare providers in recovering lost revenue.

Denial management is essential to medical billing because it ensures that healthcare providers get paid what they are owed. According to the Healthcare Financial Management Association, the average healthcare provider experiences a denial rate of 5-10% of their total claims submitted. This can cause providers to lose a lot of money, so managing denials is important in staying financially stable.
Why Accounts Receivable & Denial Management Matters!
The management of accounts receivable goes beyond mere payment collection. It is the pillar of financial health in your practice. Denied or delayed claims can accumulate rapidly, causing a flux that disturbs cash flow and affects your attention on patient care. Hence, we’ve created a comprehensive solution to counter these problems. Track uncollected payments making sure no revenue is missed.
- Study denial trends to decipher repetitive problems and devise effective preventive measures.
- Settle denied claims quickly, curtailing the time spent on appeals and corrections.
- Fast-track payment cycles to maintain a steady cash flow.
Effective Denial Management
The healthcare industry is constantly evolving, and with changes come new challenges. With the rise of high-deductible health plans and more rules from the government, it’s become common for healthcare providers to have their claims denied. The monetary impact of denied claims can be mitigated, and revenue maximized through efficient denial management.
- To identify the reason for each denial
- To reduce the cost to collect
- For a seamless integration of software and efficient workflow to prevent the future recurrence of denial
- To deal with denials within 48 hours of receipt
- To study denial trends and patterns and identify the root cause of costly denials
- To enhance the account collections and manage denials efficiently
- To reduce manual work and effort involved in checking denial errors
Comprehensive Denial Management
Claim denials are a significant hurdle for healthcare providers. Our proven denial management strategy grapples with them directly, ensuring efficient resolution and prevention.
We aim to transform denials into approvals while aiding your practice in adopting proactive strategies to decrease denial rates.
- Denial Tracking : All denied claims are logged, scrutinized, & examined to reveal underlying factors & patterns
- Appeals Handling: Our team proficiently files and tracks appeals to recover lost revenue swiftly
- Prevention Plans: We pin down denial root causes and execute corrective measures to limit future instances
The Benefits of Our Services
- Shorter Payment Cycles : Get payments quicker, shorten the time between claim submission and payment
- Lower Denial Rates : Stay ahead of denials through strategic preemptive measures
- Improved Financial Predictability : Sustain steady cash flow by superior receivable management and mitigating revenue delays
- Less Administrative Load : Let your staff focus on patient care while we handle intricate billing processes
Speak with one of our health tech experts
Our Approach to Denial Management
When it comes to dealing with denied claims, Scribe Align takes a holistic approach. To guarantee that your claims are being processed quickly and accurately, our team of specialists works together to determine the cause of denied claims, implement efficient solutions, and monitor your claims. Our goal is to help you recover the maximum possible revenue while improving your overall revenue cycle management.
Identifying the Root Cause of Denied Claims.
Identifying the root cause of denied claims is essential to take the necessary steps to correct them and reduce further denials. We will analyze the data to pinpoint where adjustments need to be made, develop strategies to combat the recurrence of the same denials and work with you to ensure that all claims are processed accurately and efficiently. This allows us to implement targeted solutions that address your specific challenges
Monitoring Claims for Maximum Efficiency
We understand the importance of accurate and prompt reimbursement, so we have established a detailed and consistent process for reviewing all claims. To keep your revenue cycle running smoothly, we employ state-of-the-art tracking technology to monitor the development of your claims and spot any potential problems ahead of time.
Can we help recover lost revenue from denied claims?
Scribe Align’s denial management services are designed to help healthcare providers recover lost revenue from denied claims. Our team of experts has a proven track record of helping providers recover lost revenue.
Awesome Return on Investment
On based of $500,000
Annual Insurance Collection
In-House Billing Cost
Prospa Charges
3% of collections for $500,000 & above

Annual Savings
$21,500
Opening & Closing Times
Mon - Sat: 8.00 am - 6.00 pm CST
Have Additional Questions?
26585 W. Agoura Rd,
Calabasas, CA 91302