Eligibility Verification
Eligibility Verification
Eligibility verification is a key part of the revenue cycle management process for medical billing. It involves checking patients’ insurance information to determine their coverage for a specific service or procedure. By performing eligibility verification, healthcare providers can ensure that they receive accurate and timely payment for their services and minimize the risk of denied or delayed claims.

Verifying a patient’s eligibility before the appointment can help reduce the number of denied claims from insurers, which can help ensure that providers receive accurate and timely payments for services rendered. Through advanced analytics and real-time data monitoring capabilities, Precision Billing Team helps healthcare providers streamline and enhance their eligibility processes, allowing them to focus on delivering the best patient care possible.
Our Eligibility & Benefits Verifications
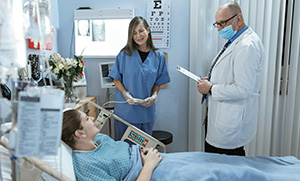
Our staff checks member eligibility with an insurance card and views detailed benefits information.
- Real-time Eligibility Verification for correct patient accounts.
- Member ID Cards Verification
- Identify the Member’s Primary Care Provider (PCP)
- Search benefits by category, including vision
- Comprehensive Fee Analysis to evade underbilling.
- Electronic Claim Submission for processing time efficiency.
- Verify the care provider’s network and tier status for the member’s plan
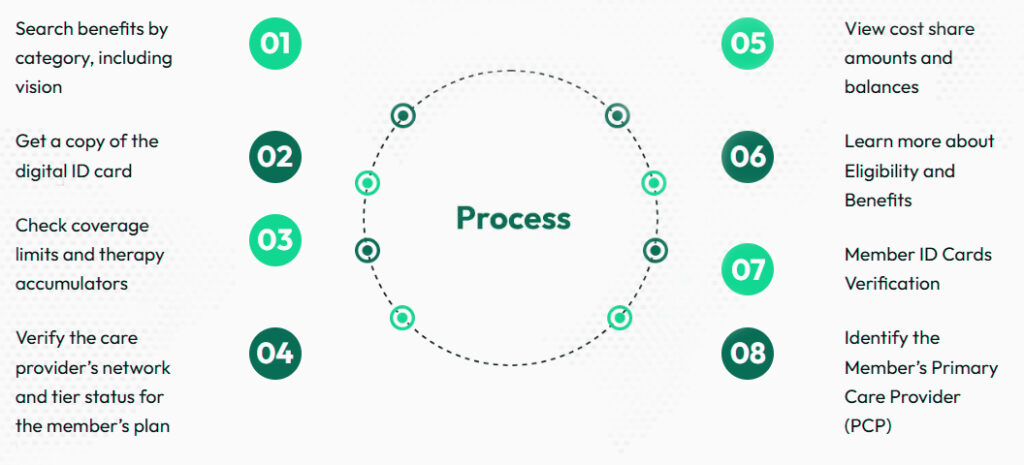
Our Eligibility Verifications Workflow
- Search benefits by category, including vision
- Get a copy of the digital ID card
- Check coverage limits and therapy accumulators
- Verify the care provider’s network and tier status for the member’s plan
- View cost-share: amounts and balances
- Learn more about Eligibility and Benefits
- Member ID Cards Verification
- Identify the Member’s Primary Care Provider (PCP)
By partnering with us, healthcare providers can enjoy a range of benefits:
- Accurate and efficient Eligibility and Benefits Verification services
- Reduced risk of denied or delayed claims
- Improved financial stability and maximum reimbursement for services
- Collection of receivables on a regular basis
- Stay up-to-date with the latest regulatory changes
- Advanced technology and a team of experts to provide tailored, personalized solutions
Speak with one of our health tech experts
Advanced technology and a team of experts to provide tailored, personalized solutions
Eligibility and Benefits Verification is confirming a patient’s insurance information and determining the coverage available for a specific service or procedure.
How can our elite task force help with Eligibility and Benefits Verification?
We offer a comprehensive and efficient solution for Eligibility and Benefits Verification. Our team of experts uses advanced technology to verify insurance information accurately and quickly, and our tailored, personalized services can help healthcare providers maximize their financial performance.
Why choose our team?
- Regular QA checking
- Dedicated project manager
- Regular and stat turnaround times
- No set-up fees or long-term contracts
- Daily, weekly, and monthly status reports
- We can work on your software
Awesome Return on Investment
On based of $500,000
Annual Insurance Collection
In-House Billing Cost
Prospa Charges
3% of collections for $500,000 & above

Annual Savings
$21,500
Opening & Closing Times
Mon - Sat: 8.00 am - 6.00 pm CST
Have Additional Questions?
26585 W. Agoura Rd,
Calabasas, CA 91302